OVERVIEW
A cerebral or intracranial aneurysm is an abnormal focal dilation of an artery in the brain that results from a weakening of the inner muscular layer (the intima) of a blood vessel wall. The vessel develops a “blister-like” dilation that can become thin and rupture without warning. The resultant bleeding into the space around the brain is called a subarachnoid hemorrhage (SAH). This kind of hemorrhage can lead to a stroke, coma and/or death.
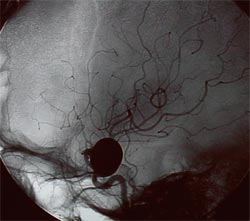
Aneurysms are usually found at the base of the brain just inside the skull, in an area called the subarachnoid space. In fact, 90 percent of SAHs are attributed to ruptured cerebral aneurysms and the two terms are often used synonymously.
Aneurysms range in size, from small – about 1/8 inch – to nearly one inch. Aneurysms larger than one inch are called giant aneurysms, pose a particularly high risk and are difficult to treat. The exact mechanisms by which cerebral aneurysms develop, grow and rupture are unknown.
However, a number of factors are believed to contribute to the formation of cerebral aneurysms, including:
- Hypertension (high blood pressure)
- Cigarette smoking
- Congenital (genetic) predisposition
- Injury or trauma to blood vessels
- Complication from some types of blood infections
Patients with intracranial aneurysms can present with SAH from aneurysmal rupture or with un-ruptured aneurysms, which may have been discovered incidentally or resulted in neurological symptoms. An aneurysm ruptures when a hole develops in the sac of the aneurysm. The hole can be small, in which case only a small amount of blood leaks, or large, leading to a major hemorrhage. An un-ruptured aneurysm is the one whose sac has not previously leaked. Every year approximately 30,000 patients in the U.S. suffer from a ruptured cerebral aneurysm, and up to 6 percent of the population may have an un-ruptured cerebral aneurysm.
A series of 111 patients with un-ruptured aneurysms showed:
- 51 percent with asymptomatic aneurysms
- 17 percent with acute symptomatology — such as ischemia (37% of aneurysms)
- Headache (37 percent of aneurysms)
- Seizures (18 percent of aneurysms)
- Cranial neuropathies (12 percent of aneurysms)
- Chronic symptomatology (32 percent) which included headache (51%)
- Visual deficits (29 percent)
- Weakness (11 percent) and
- Facial pain (nine percent)
The management of both ruptured and un-ruptured cerebral aneurysms poses a significant challenge for patients and their treating physicians (1).
TREATMENT + CARE
There is little doubt on the treatment for ruptured cerebral aneurysms, which are typically secured with clips or coils to prevent re-rupture. Occasionally if the patients’ neurological status is poor on presentation, they have multiple medical co-morbidities, especially in the elderly age group, and the chances of significant recovery seem low, the treating physician may not recommend aggressive management. The ‘Hunt and Hess grading scale,’ introduced in 1968, is generally used at most neurosurgical centers to classify the severity of SAH based on the patient’s clinical condition.
The worse the patients’ neurological status, the higher is the grade (2):
- Asymptomatic, mild headache, slight nuchal rigidity (neck stiffness)
- Moderate to severe headache, nuchal rigidity, cranial nerve palsy, no other neurological deficit
- Drowsiness / confusion, mild focal neurologic deficit
- Stupor, moderate-severe hemiparesis
- Coma, extensor posturing
The treatment for un-ruptured cerebral aneurysms has been a matter of debate for decades. In the largest study on the management of un-ruptured aneurysms “International study of unruptured intracranial aneurysms” (ISUIA), the five-year cumulative rupture rates for patients without a history of SAH and with aneurysms in anterior circulation were 0 percent, 2.6 percent, 14.5 percent and 40 percent for aneurysms <7 mm, 7–12 mm, 13–24 mm, and > 25 mm, respectively.
For posterior circulation and posterior communicating artery aneurysms these rates were higher: 2.5 percent; 14.5 percent, 18.4 percent and 50 percent for <7 mm, 7–12 mm, 13–24 mm, and > 25 mm, respectively. The study suggested that aneurysms < 7 mm in the anterior circulation have 0.05 percent risk of rupture and should be observed. This study could not make recommendations regarding the modality of treatment because the characteristics of patients in the endovascular cohort differed greatly from those in the surgical group (3).
This study has been criticized for selection bias and study design. In clinical practice SAH from aneurysms smaller than 7 mm is not infrequently encountered. Over the years a number of factors have been reported which can influence rupture rates of the aneurysms. Factors such as family history of intracranial aneurysms, history of smoking, excessive alcohol consumption, female sex, previous SAH, symptomatic aneurysm, its location and size have shown negative correlations. Besides these factors, a patient’s life expectancy and medical co-morbidities are also taken into account with discussing the management options (4).
In 2007, based on the critical analysis of the literature available at that time Komotar et al (4) recommended that:
- with rare exceptions, all symptomatic un-ruptured aneurysms should be treated;
- small, incidental aneurysms less than 5 mm in diameter should be managed conservatively in virtually all cases;
- aneurysms larger than 5 mm in patients younger than 60 years of age should be seriously considered for treatment;
- large, incidental aneurysms larger than 10 mm should be treated in nearly all patients younger than 70 years of age.
Broadly, three treatment options for people with the diagnosis of cerebral aneurysm include:
- medical (non-surgical) therapy
- surgical therapy or clipping and
- endovascular therapy or coiling with or without adjunctive devices
Medical Therapy
Medical therapy is usually only an option for the treatment of un-ruptured intracranial aneurysms. Strategies include smoking cessation and blood pressure control. These are the only factors that have been shown to have a significant effect on aneurysm formation, growth and/or rupture. Both patient and doctor can work together to design an individualized smoking cessation program that is both practical and feasible for the patient’s lifestyle. In addition, if suffering from high blood pressure, the doctor may choose to start you on an anti-hypertensive (blood pressure lowering) medication and/or diet and exercise program. Finally, periodic radiographic imaging (either MRA, CT scan or conventional angiography) may be recommended at intervals to monitor the size and/or growth of the aneurysm. Because the mechanisms of aneurysm rupture are incompletely understood, and because even aneurysms of very small size may rupture, the role of serial imaging for cerebral aneurysm is undefined.
Surgical Clipping
In 1937, Walter Dandy, MD, a famous American neurosurgeon, introduced the method of “clipping” an aneurysm when he applied a V-shaped, silver clip to the neck of an internal carotid artery aneurysm. Since that time, aneurysm clips have evolved into hundreds of varieties, shapes and sizes. The mechanical sophistication of available clips, along with the advent of the operating microscope in the 1960s have made surgical clipping the gold standard in the treatment of both ruptured and un-ruptured cerebral aneurysms. In spite of these advances, surgical clipping remains an invasive and technically challenging procedure.
How is an Aneurysm Surgically Clipped?
An aneurysm is clipped through a craniotomy, which is a surgical procedure in which the brain and the blood vessels are accessed through an opening in the skull. After the aneurysm is identified, it is carefully dissected (separated) from the surrounding brain tissue. A small metal clip (usually made from titanium) is then applied to the neck (base) of the aneurysm. Aneurysm clips come in all different shapes and sizes, and the choice of a particular clip is based on the size and location of an aneurysm. The clip has a spring mechanism which allows the two “jaws” of the clip to close around either side of the aneurysm, thus occluding (separating) the aneurysm from the parent (origin) blood vessel. In the ideal clipping, normal blood vessel anatomy is physically restored by excluding the aneurysm sac from the cerebral circulation.
Endovascular Coiling
Endovascular techniques for treating aneurysms date back to the 1970s with the introduction of proximal balloon occlusion by Fjodor A. Serbinenko, MD, a Russian neurosurgeon. During the 1980s, endovascular treatment of aneurysms with balloon occlusions was associated with high procedural rate of rupture and complications. Guido Guglielmi, MD, an American-based neuroradiologist, invented the platinum detachable microcoil, which was used to treat the first human being in 1991. The development of Guglielmi detachable coils (GDCs), and their FDA approval in 1995, revolutionized endovascular treatment of cerebral aneurysms.
How is an Aneurysm Endovascularly Coiled?
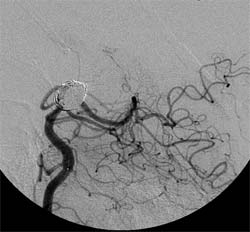
The common goal of both surgical clipping and endovascular coiling is to eliminate blood flow into the aneurysm. Efficacy (long-term success or effectiveness of the treatment) is measured by evidence of aneurysm obliteration (failure to be demonstrated by conventional or noninvasive angiography), without evidence of recanalization (any blood flow into the aneurysm) or recurrence (reappearance).
Guglielmi detachable coils, known as GDCs, are soft wire spirals originally made out of platinum. These coils are deployed (released) into an aneurysm via a microcatheter that is inserted through the femoral artery of the leg and carefully advanced into the brain. The microcatheter is selectively advanced into the aneurysm itself, and the microcoils are released in a sequential manner. Once the coils are released into the aneurysm, the blood flow pattern within the aneurysm is altered, and the slow or sluggish remaining blood flow leads to a thrombosis (clot) of the aneurysm. A thrombosed aneurysm resists the entry of liquid blood, providing a seal in a manner similar to a clip.
Endovascular coiling is an attractive option for treating aneurysms because it does not require opening of the skull, and is generally accomplished in a shorter time frame, which lessens the anesthesia given. Nevertheless, important differences remain between clipping and coiling, including the nature of the seal created. Because coiling does not physically re-approximate the inner blood vessel lining (endothelium), recanalization may occur through the eventual compaction of the coils into the aneurysm by the bloodstream.
One of the largest, randomized controlled trials comparing surgical clipping and endovascular coiling — International Subarachnoid Aneurysm Trial (ISAT) — randomly allocated the patients to either neurosurgical clipping or endovascular coiling after a SAH. In the first report published in 2002, 2,143 participants were enrolled and randomly assigned to the endovascular coiling group and the surgical clipping group. They concluded that survival (free of disability) at one year was better with endovascular coiling. Long-term risk of further bleeding from treated aneurysm was low with either therapy, but higher with endovascular coiling, as compared to surgical clipping (5).
The investigators recently published the long-term outcomes from 1,644 patients enrolled from 22 U.K. neurosurgical centers who were followed up for 10–18.5 years for death and clinical outcomes. At long-term follow-up rates of increased dependency alone did not differ between groups, the probability of death or dependency was significantly greater in the neurosurgical group and re-bleeding was more likely after endovascular coiling (6).
However, this study, like many other stroke trials, has many shortcomings and should be interpreted with caution (7). Meta-analyses of randomized trials comparing endovascular coiling and surgical clipping (including ISAT) conducted later were unable to show a significant difference between endovascular treatment and neurosurgical clipping in mortality and reported that endovascular treatment was associated with higher rates of re-bleeding (8, 9).
Often endovascular coiling may need to be performed with stent — or balloon assistance — for complex aneurysms such as wide-necked aneurysms with lower dome-to-neck ratios, large and giant aneurysms. Stent — or balloon-assisted coiling — is done to prevent herniation of the coil mass into the parent artery which can result in stroke. For balloon-assisted coiling, the balloon is temporarily inflated at the neck of the aneurysm while the coils are placed into the aneurysm. For stent-assisted coiling, the stent is permanently placed across the aneurysm neck. There are advantages and disadvantages of both approaches.
The patients who have the stent placed need to be on anti-platelets medications, limiting their use in ruptured aneurysms, although stent-assisted coiling has been used in ruptured aneurysms with good outcomes. Stents have also been shown to reduce aneurysm recanalization and result in further occlusion of incompletely coiled aneurysms (10, 11). A literature review on stent-assisted coiling in 2012 reported the overall complication rate of 19 percent with an overall death rate of 2.1 percent (12).
Flow Diversion
Flow diverter (FD) stents were introduced about 7 years ago into the clinical armamentarium of the neuro-interventionists as an additional tool for aneurysm treatment. They have higher metal surface area coverage (about 30-35 percent) as compared to the previous generation stents which have about 8-10 percent metal surface-area coverage (13).
FDs are tubular stent-like implants with a low porosity (metal-free to metal-covered area) and a high pore density with two main work mechanisms (14):
- Flow diversion: As the name indicates, FDs bridge the aneurysm neck and divert the blood flow away from the aneurysm sac, due to impedance created by the mesh of the implant. Reduction of the blood flow into the aneurysmal sac causes stasis of blood flow within the aneurysm which then leads to an inflammatory response followed by thrombosis and “healing” of the aneurysm.
- Endoluminal reconstruction of the parent artery: The FD provides a scaffold for neo-endothelialization across the aneurysm neck and results in endoluminal reconstruction of the parent artery excluding the aneurysm from the circulation.
FD stents clinically available at the current time include:
- Pipeline Embolization Device (EV3-MTI, Irvine, CA)
- Silk (Balt, Montmorency, France)
- Surpass (Stryker, Fremont, CA)
- Flow Redirection Endoluminal Device (FRED) (Microvention, Tustin, CA)
Pipeline embolization device (PED) is currently used most often in the U.S. and most of the literature on flow-diversion for intracranial aneurysms is based on its use. The PED is a flexible microcatheter-delivered self-expanding cylindric construct composed of 48 braided strands of cobalt chromium and platinum. The Food and Drug Administration (FDA) approved the PED for the treatment of large or giant wide-necked intracranial aneurysms from the petrous to the superior hypophyseal segments of the internal carotid artery (ICA), which is a section of the artery that supplies the blood to the brain. (15) Over the last few years, PED has also been used beyond the FDA approved indications as an “off-label device” with good outcomes. (16)
The concept behind the treatment is the same with all four FDs. Flow diversion is generally performed for the treatment of aneurysms that are challenging and less amenable to traditional endovascular coiling; such as complex aneurysms, including large and giant aneurysms, wide-neck aneurysms, fusiform aneurysms and recanalized aneurysms after previous coiling. Stent-assisted coiling and balloon-assisted coiling are alternative endovascular options for such aneurysms; however, some studies reported their limited efficacy due to high recanalization rates (12).
Dual antiplatelet therapy with Plavix (Clopidogrel) and aspirin (ASA) is recommended starting prior to the placement of the device and continued afterwards for three to six months followed by aspirin monotherapy lifelong. That is why most aneurysms treated are un-ruptured although there are cases where they were used for ruptured aneurysms also. Most centers still limit their use to the un-ruptured aneurysms. For adequate anticoagulation (and to lower the thromboembolic complications) prior to device placement, Plavix assays are checked at baseline before the administration of Plavix and then again just before the procedure. The percentage of inhibition is calculated and the dosage is adjusted to achieve adequate platelet inhibition before the procedure. Patients with resistance to Plavix are switched to a different anti-platelet drug.
After the routine groin access and placement of a sheath, the microcatheter is navigated inside the larger guide catheter to the desired position across the aneurysm neck. FD stent is then passed through the microcatheter and deployed across the aneurysm neck carefully under the angiographic guidance.
The coils don’t need to be packed as tightly, if at all, as in traditional aneurysmal coiling, which decreases the chances of mass effect from the large aneurysms (14). The results from the large retrospective and prospective single- and multi-center studies have shown an excellent feasibility of the treatment with a high efficacy and acceptable periprocedural complications (occurring soon before, during or after the performance of a medical procedure) as well as morbidity and mortality rates (17,18).
Besides the important complications such as thromboembolic events and the intra-procedural aneurysm rupture, which are also seen with traditional aneurysm coiling, other complications seen with the use of FDs include delayed aneurysmal rupture causing hemorrhage and distant (away from aneurysm) intraparenchymal hemorrhage. The mechanisms for delayed hemorrhage and distant intraparenchymal hemorrhage are not well understood. The hypotheses suggested include the inflammation associated with thrombus formation weakens the aneurysmal wall causing rupture or the hemodynamic changes within the aneurysm causing stress and rupture (14).
From the Retrospective Analysis of Delayed Aneurysm Ruptures (RADAR) study analysis, delayed aneurysms rupture after FDs use occurred in 1.0 percent of patients and delayed parenchymal hemorrhage was reported in 1.9 percent of patients (19).
Flow Disruption
Intrasaccular flow disruption with a WEB device is one of the latest technological advancements in management of wide-necked aneurysms especially at the bifurcation of an artery. The WEB device is placed within an aneurysm in contrast to the FDs which are placed in the parent artery. One of the biggest advantages is the reduced need for antiplatelet medications, especially for the ruptured aneurysms, which is particularly helpful in patients with SAH. The clinical experience with its use is currently limited; however, the preliminary retrospective multicenter series reported 100 percent technical feasibility, 4.8 percent morbidity and 0 percent mortality (20). The WEB device is not FDA-approved in the United States.
Who Performs the Procedure?
Surgical clipping of a cerebral aneurysm is always performed by a neurosurgeon, often one with expertise in cerebrovascular disease. Most cerebrovascular neurosurgeons have had five to seven years of general neurosurgery training and an additional one to two years of specialized cerebrovascular training.
Endovascular coiling is done either by a neurosurgeon or by an interventional neuroradiologist. An interventional radiologist has undergone extensive training (three to five years) in both radiology and interventional (invasive) procedures involving the brain and spinal cord. All neurosurgeons that perform endovascular coiling have undergone additional training in endovascular techniques in addition to full neurosurgery training (five to seven years of residency).
Safety and Common Complications
Although the frequencies of certain complications vary according to the intervention, both clipping and coiling share the same complications. Rupture of the aneurysm is one of the most serious complications seen in either procedure. Exact frequencies of ruptures are not well documented, but reported rupture rates range from 2 percent to 3 percent for both coiling and clipping. Rupture can cause massive intracerebral hemorrhage (hemorrhagic stroke or bleeding into the brain) and subsequent coma or death. Although rupture can have catastrophic consequences during either procedure, surgery probably provides a better opportunity to control hemorrhage because of direct access to the ruptured aneurysm and the supplying vessels.
Ischemic stroke (stroke secondary to decreased blood oxygen) is another serious complication frequently encountered in both clipping and coiling. The pattern and distribution of strokes varies according to the aneurysm location and procedure type.
The actual length of the procedure, the associated risks, the projected recovery time and the expected prognosis (outcome) depend on both the location of the aneurysm, the presence/severity of hemorrhage and the patient’s underlying medical condition. Therefore, each individual case should be discussed with the treating neurosurgeon/physician.
How Do I Decide What Procedure to Have if I Have a Cerebral Aneurysm?
The treatment of choice for an intracranial aneurysm, like all medical decisions, should be agreed upon by both the physician and the patient. In the case of either ruptured or un-ruptured intracranial aneurysms, the treating physician should discuss the risks and benefits of each available treatment option. The physician will usually make recommendations for one treatment over another, depending on the facts of each individual case. Seeking a second opinion, when possible, is usually advisable.
Although unresolved controversies remain as to what the best treatment option is for an individual patient, both surgical clipping and endovascular coiling/stenting are considered to be viable treatment options in the management of cerebral aneurysms today.
RESOURCES
SOURCES
- Raps EC, Rogers JD, Galetta SL, Solomon RA, Lennihan L, Klebanoff LM, Fink ME: The clinical spectrum of unruptured intracranial aneurysms. Arch Neurol 50:265–268, 1993.
- Hunt WE, Hess RM. “Surgical risk as related to time of intervention in the repair of intracranial aneurysms.” Journal of Neurosurgery 1968 Jan;28(1):14-20.
- Wiebers DO, Whisnant JP, Huston J 3rd, Meissner I, Brown RD Jr, Piepgras DG, Forbes GS, Thielen K, Nichols D, O’Fallon WM, Peacock J, Jaeger L, Kassell NF, Kongable-Beckman GL, Torner JC; International Study of Unruptured Intracranial Aneurysms Investigators. Unruptured intracranial aneurysms: natural history, clinical outcome, and risks of surgical and endovascular treatment. Lancet. 2003 Jul 12;362(9378):103-10.
- Komotar RJ, Mocco J, Solomon RA.Guidelines for the surgical treatment of unruptured intracranial aneurysms: the first annual J. Lawrence pool memorial research symposium–controversies in the management of cerebral aneurysms. Neurosurgery. 2008 Jan;62(1):183-93; discussion 193-4.
- Molyneux A, Kerr R, Stratton I, Sandercock P, Clarke M, Shrimpton J, Holman R; International Subarachnoid Aneurysm Trial (ISAT) Collaborative Group. International Subarachnoid Aneurysm Trial (ISAT) of neurosurgical clipping versus endovascular coiling in 2143 patients with ruptured intracranial aneurysms: a randomised trial. Lancet. 2002 Oct 26;360(9342):1267-74.
- Molyneux AJ, Birks J, Clarke A, Sneade M, Kerr RS.The durability of endovascular coiling versus neurosurgical clipping of ruptured cerebral aneurysms: 18 year follow-up of the UK cohort of the International Subarachnoid Aneurysm Trial (ISAT) Lancet. 2014 Oct 28. pii: S0140-6736(14)60975-2.
- Ajith J Thomas, Christopher S Ogilvy. ISAT: equipoise in treatment of ruptured cerebral aneurysms? Lancet. 2014 Oct 28. pii: S0140-6736(14)61736-0.
- Lanzino G, Murad MH, d’Urso PI, Rabinstein AA. Coil embolization versus clipping for ruptured intracranial aneurysms: a meta-analysis of prospective controlled published studies. AJNR Am J Neuroradiol 2013; 34: 1764–68.
- Li H, Pan R, Wang H, et al. Clipping versus coiling for ruptured intracranial aneurysms: a systematic review and meta-analysis. Stroke 2013; 44: 29–37.
- Lawson MF, Newman WC, Chi YY, Mocco JD, Hoh BL. Stent-associated flow remodeling causes further occlusion of incompletely coiled aneurysms.Neurosurgery. 2011 Sep;69(3):598-603; discussion 603-4.
- Fargen KM, Hoh BL, Welch BG, Pride GL, Lanzino G, Boulos AS, Carpenter JS, Rai A, Veznedaroglu E, Ringer A, Rodriguez-Mercado R, Kan P, Siddiqui A, Levy EI, Mocco J. Long-term results of enterprise stent-assisted coiling of cerebral aneurysms. Neurosurgery. 2012 Aug;71(2):239-44; discussion 244.
- Shapiro M, Becske T, Sahlein D, Babb J, Nelson PK. Stent-supported aneurysm coiling: a literature survey of treatment and follow-up. AJNR Am J Neuroradiol. 2012;33:159–163.
- Nelson PK, Lylyk P, Szikora I, Wetzel SG, Wanke I, Fiorella D.The pipeline embolization device for the intracranial treatment of aneurysms trial. AJNR Am J Neuroradiol. 2011 Jan;32(1):34-40.
- Pierot L, Wakhloo AK. Endovascular treatment of intracranial aneurysms: current status. Stroke. 2013 Jul;44(7):2046-54.
- Kan P, Siddiqui AH, Veznedaroglu E, Liebman KM, Binning MJ, Dumont TM, Ogilvy CS, Gaughen JR Jr, Mocco J, Velat GJ, Ringer AJ, Welch BG, Horowitz MB, Snyder KV, Hopkins LN, Levy EI. Early postmarket results after treatment of intracranial aneurysms with the pipeline embolization device: a U.S. multicenter experience. Neurosurgery. 2012 Dec;71(6):1080-7; discussion 1087-8.
- Kulcsár Z, Wetzel SG, Augsburger L, Gruber A, Wanke I, Rüfenacht DA. Effect of flow diversion treatment on very small ruptured aneurysms. Neurosurgery. 2010 Sep;67(3):789-93.
- Piano M1, Valvassori L, Quilici L, Pero G, Boccardi E. Midterm and long-term follow-up of cerebral aneurysms treated with flow diverter devices: a single-center experience.J Neurosurg. 2013 Feb;118(2):408-16.
- O’Kelly CJ, Spears J, Chow M, Wong J, Boulton M, Weill A, et al. Canadian experience with the pipeline embolization device for repair of unruptured intracranial aneurysms. AJNR Am J Neuroradiol. 2013;34:381–387.
- Kulcsar Z, Szikora I. The ESMINT Retrospective Analysis of Delayed Aneurysm Ruptures after flow diversion (RADAR) study. EJMINT. 2012.
- Pierot L, Liebig T, Sychra V, Kadziolka K, Dorn F, Strasilla C, et al. Intrasaccular flow disruption: a new endovascular approach for the treatment of intracranial aneurysms. Results of a preliminary clinical evaluation in a multicenter series. AJNR Am J Neuroradiol. 2012;33:1232–1238.
Note from AANS
The AANS does not endorse any treatments, procedures, products or physicians referenced in these patient fact sheets. This information is provided as an educational service and is not intended to serve as medical advice. Anyone seeking specific neurosurgical advice or assistance should consult his or her neurosurgeon, or locate one in your area through the AANS’ Find a Board-certified Neurosurgeon online tool.
